Lipedema is a progressive condition primarily affecting the distribution of adipose tissue in the body, causing disproportionate fat accumulation, particularly in the legs, hips, bum and sometimes arms. While it’s generally characterised by adverse physical symptoms, it’s important to understand the link between Lipedema and eating disorders. It’s arguably one of the most important topics in the Lipedema community and isn’t spoken about enough, yet the connection between the two is so apparent.
In this blog, I will include testimonies from various women discussing their experiences with Lipedema and eating disorders. I have chosen to keep their identities anonymous by using fictitious names to protect their privacy. Some of the content mentioned may be triggering for anyone currently suffering from an eating disorder, so please bare this in mind.
Understanding Lipedema
Lipedema is often misunderstood and misdiagnosed as obesity, cellulite or Lymphedema due to its aesthetic similarities. It’s thought to be hereditary and affects predominantly women, leading to an abnormal buildup of fat tissue in certain areas of the body. The fat distribution, especially in the earlier Lipedema stages, is often described as having a ‘pear-shaped’ figure or a ‘column-like’ appearance to the legs.
Understanding Eating Disorders
Eating disorders, on the other hand, are mental health conditions characterised by problematic eating patterns and attitudes towards food and body image. Common eating disorders include anorexia nervosa, bulimia nervosa, and binge-eating disorder.
The Link Between Lipedema and Eating Disorders
A study consisting of 100 patients with Lipedema found that 74% had a history of eating disorders, 12% had periodic binge eating attacks, 8% had bulimia and 16% had anorexia nervosa.
When we consider that the average percentage of women with an eating disorder globally is around 10%, the glaringly obvious link between Lipedema and eating disorders becomes more obvious.
In my opinion, the constant cycle of restricting food intake for women with Lipedema derives from the fact that we struggle to lose Lipedema fat with traditional diet and exercise methods. Lipedema tissue does not respond in the same way as ‘normal’ fat, therefore we resort to extreme measures when we do not see the results we so desperately crave.
Contributing Factors
- Body Image:
Lipedema can significantly alter a woman’s body shape and lead to feelings of self-consciousness and body dissatisfaction. This altered body image often contributes to the development or exacerbation of eating disorders.
- Weight Management:
Women with Lipedema often struggle with managing their weight despite efforts to maintain a healthy lifestyle. This frustration may lead to extreme dieting or other disordered eating habits.
- Misdiagnosis:
Lipedema is frequently misdiagnosed, leading women to seek alternative explanations for their symptoms, including turning to restrictive diets or excessive exercise to control their weight.
- Emotional Impact:
Coping with the chronic discomfort and physical changes in the body associated with Lipedema can be emotionally challenging. This emotional distress may increase vulnerability to developing eating disorders as a way to cope with difficult feelings and emotions.
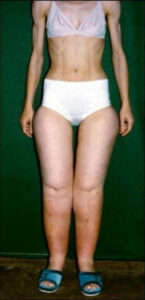
The above image shows a woman suffering from Lipedema and Anorexia Nervosa.
My Experience with Lipedema and Eating Disorders
I think I’ve only really come to terms with my disordered eating habits in the past since getting my Lipedema diagnosis in December 2022. Something clicked and I realised that a period of extremely restrictive eating at the age of 19 was exacerbated by my Lipedema, as well as various other factors.
In my teens, I was very slim but at the age of 15 when I started the contraceptive pill, the legs began to balloon, especially around the ankles and knees. That is where my disordered eating began, I would eat a tiny bowl of Special K cereal at college every day instead of a healthy, balanced meal.
This then compounded in my second year of university after a close family member passed away very suddenly, and my relationship with my boyfriend at the time broke down. It felt like my whole world was collapsing and I fell into a pattern of seriously restricting my daily food intake. At my worst, I ate one small jacket potato per day with cream cheese. The weight literally fell off me in a matter of weeks. For reference, I’m 5’6” and I weighed around 8 stone.
I remember at a house party, I opened the door to one of my close friends and she gasped when she saw me and tiny, sparrow-like frame. Everyone kept commenting on how much weight I’d lost, but I couldn’t see it myself. My main frustration was that no matter how ‘skinny’ I was, my legs were still ‘column-like’ with no definition at the knees or ankles.
I know Lipedema wasn’t the main cause for my disordered eating, however it definitely didn’t help. I’m now realising that this is the case for so many women with Lipedema, the inability to lose much Lipedema tissue means that we resort to severe eating restrictions, which is actually more detrimental to our Lipedema symptoms than eating a ‘normal’ diet.
Left: Aged 19 during a period of restricted eating. Right: Aged 25 once recovered.
“Fighting the Family Hips”
For some women with Lipedema, their disordered eating began during early adolescence. When overt signs of Lipedema showed in Suzanne’s arms and legs at age 12, her parents – who were unaware of her condition – put her on a diet.
“There was a lot of talk about, ‘Fighting the family hips,’” said Suzanne, who now believes from her own diagnosis that her two sisters also have Lipedema.
Suzanne continued to restrict her eating into adulthood. “It got gradually worse and worse,” she admitted. At her lowest point, she was consuming only 800 calories a day.
Society’s obsession with thinness leads girls and women with Lipedema to starve themselves, or binge and purge, because simply eating a healthy diet won’t radially change the thickness of their limbs.
“I got smaller, but the issues I had with proportion in my legs and arms didn’t go away,” Suzanne clarified. “You could literally count my ribs, but I still couldn’t wear shorts without terror because of my ‘fat legs.’”
Like Suzanne, Olivia had no idea she had Lipedema when her brother made fun of her as a teen for having large legs. “It was the 2000s, so think legs in skinny jeans were in,” she said. “The looks at the time were flowy on top and tight on the bottom – the most uncomfortable and unflattering thing for a girl with Lipedema.”
Olivia had a short-lived eating disorder at age 17, and then maintained disordered eating habits for around a decade. This is unfortunately the case for so many women suffering with both conditions.
When Claire was in her early 20s, she would go for days without eating. “I didn’t know I had Lipedema when I was trying to starve myself,” she shared. “I just thought I was fat.”
Claire received a wake-up call when she fainted in the shower after four straight days of fasting. “I got spooked and went back to eating ‘normally.’” she said.
However, during her early 40s, she embarked on a series of fad diets and over-the-counter pills. “I got really depressed, thinking there must be something seriously wrong with me,” Claire admitted.
Seeking Professional Help
If all of this sounds familiar and you suspect you suffer from Lipedema and an eating disorder, or someone you know does, it’s crucial to seek professional help. Both Lipedema and eating disorders are complex conditions that require specialised care and treatment.
Simply knowing they have Lipedema can help so many women in their recovery from disordered eating. Suzanne was in recovery when she was diagnosed with Lipedema.
“I understand now that my body has a condition that is separate from how much I work out or eat,” she said, noting this prevents her from relapsing. “Now my focus is on being and eating healthy, without so much preoccupation with eliminating cellulite.”
When Claire finally discovered she had Lipedema at age 50, she felt relieved. “I finally found what was so seriously wrong with me, why I could only get to a certain point in my weight loss,” she said. “I’m certainly kinder to myself. I don’t beat myself up like I used to. My depression lows aren’t as low.”
Olivia’s Lipedema ‘diagnosis’ came from a plastic surgeon, but she said it’s clear visually and palpating her legs that she has the condition. “I do think just realizing I had Lipedema helped me develop a healthier relationship with food,” she stated.
Unfortunately for us, the lack of awareness and support for women with Lipedema makes diagnosis extremely difficult. So much more needs to be done. The healthcare system seems to have failed us. I hope in the coming years Lipedema will be recognised as the life altering condition that it is.
If you have, or suspect you have Lipedema, consulting with a knowledgeable Lipedema specialist who understands the condition is essential for proper diagnosis and management. An anti-inflammatory diet, MLD massages, wearing Lipedema compression garments and other conservative measures can help control Lipedema symptoms and improve day to day life.
If you’re also struggling with an eating disorder, reaching out to a mental health professional or eating disorder specialist is critical. Treatment may involve therapy, nutritional counselling, and in some cases, medical intervention.
An Overview of Lipedema and Eating Disorders
Lipedema and eating disorders is a topic that is currently unexplored. Studies show that there is an undeniable connection, so there needs to be more awareness for the women that are struggling with both conditions.
I hope this blog sheds light on the uphill battle of women, like myself, who try to manage their Lipedema symptoms day in, day out. Lack of awareness around the causes and symptoms of Lipedema has led so many of us to punish ourselves with severely restrictive or binge eating.
Please remember, this is not your fault. In the majority of cases, Lipedema is hereditary or caused by hormonal factors. Educate yourself on conservative measures for Lipedema rather than blaming yourself for something completely out of your control.
Help Us Understand More
Lipedema and eating disorders are closely linked, yet there’s still so much to learn. If you have Lipedema, please take a moment to fill out this quick anonymous survey to help gather important data on this connection.
Your input could make a real difference in raising awareness and improving understanding.
Disclaimer: My blogs talk about Lipedema, diet, surgery and much more. I’m talking from my point of view to help women, and remind them they are not alone. I am not a medical professional, so the content above is from my own perspective with research I have done into the topic. It’s not meant as medical advice, you should always consult your doctor or a specialist for both your diagnosis, and a treatment plan.





I have had Lipedema all my life, I was put on a diet from 2, I can’t eat apples again as I was force fed them being the fat kid. My paternal nana and aunts have lipedema some always and others it’s been triggered later, I have disordered eating, when I got diagnosed age 50, the clinic I go to is in a hospice which made me think completely differently as how many people my age drive up that road to the clinic and never go back down it? So it gave me a completely different perspective. I am riddled with lipedema legs, bum, tum, arms & back I don’t have the body I have disordered ate for and I have a chronic condition but I do have a body that works and whilst it’s a cruel disease, I dress my lipedema well and live my life to the fullest. My relationship with food has changed since my diagnosis it’s much better as I know the odds have always been against me, I feel much better about myself now since being diagnosed. I am hoping the menopause is kind to me as if not surgery will have to be an option but currently I am trying alternative methods to avoid surgery.